TL;DR:
- Hair loss diagnosis requires comprehensive evaluation including scalp exams, blood tests, and biopsies.
- Treatments vary based on specific conditions, with evidence supporting medications like minoxidil and finasteride.
- Monitoring hair health objectively between visits enhances treatment effectiveness and outcomes.
You've tried the shampoos. You've ordered the supplements. You've watched the tutorials. And yet, every morning the drain tells a different story. The frustrating truth is that most people treat hair loss like a single problem with a single fix, when in reality it's a symptom with dozens of possible causes. A qualified hair dermatologist doesn't just look at your scalp; they decode it. This guide walks you through exactly what that process looks like, what treatments actually work, and how to make the most of your specialist visits so you stop guessing and start seeing real results.
Table of Contents
- What does a hair dermatologist do?
- How hair loss is diagnosed: Step-by-step process
- Treatment options: What to expect from a hair dermatologist
- Targeted solutions for unique types of hair loss
- Our take: Why measuring your hair health is as vital as the right dermatologist
- Take the next step: Tools and clinics for measurable progress
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Expert diagnosis matters | Seeing a hair dermatologist is crucial for an accurate diagnosis and effective treatment plan. |
| Treatments are personalized | The best results come from therapies tailored to your exact type of hair loss. |
| Track your progress | Measuring your hair health visibly and with tools leads to better long-term outcomes. |
| Emerging therapies exist | Advanced options like JAK inhibitors and AI-powered analysis can help when traditional treatments fail. |
What does a hair dermatologist do?
Hair dermatologists are medical doctors who specialize in conditions affecting the skin, scalp, and hair follicles. They go far beyond what a general practitioner or a trichologist (a non-medical hair specialist) can offer. Their training includes both systemic medicine and hands-on scalp diagnostics, which means they can connect the dots between your bloodwork, your lifestyle, and what's happening at follicle level.
One thing people often get wrong is assuming that any professional offering a "hair consultation" carries the same qualifications. Salons, wellness centers, and even some online clinics market hair loss services, but they can't order lab tests, perform biopsies, or prescribe medications. Only a board-certified dermatologist can do all of that in one visit.
Local expertise also matters more than you might expect. Dermatologists who practice in your region often see patterns tied to local water quality, climate, and even genetic populations. A dermatologist in a hard-water area, for example, will be familiar with how mineral buildup stresses the scalp and may ask questions about your water source as part of the intake process.
Here is what a comprehensive hair dermatologist assessment typically covers:
- Medical history: Previous diagnoses, medications, nutritional status, and family hair loss patterns
- Physical examination: Visual scalp inspection, hair pull test (to assess shedding rate), and hairline mapping
- Trichoscopy: A dermoscopy or trichoscopy tool magnifies the scalp up to 70 times, revealing follicle miniaturization, scaling, and vascular patterns invisible to the naked eye
- Blood tests: Ferritin, thyroid panel (TSH, T3, T4), vitamin D, zinc, and androgens are common targets
- Scalp biopsy: Reserved for uncertain or scarring cases, this provides a tissue-level diagnosis
"A dermatologist who skips the pull test and jumps straight to selling you a treatment program is a red flag. Diagnosis always comes before prescription."
Pro Tip: Before your first appointment, photograph your scalp in good lighting every two weeks for a month. This gives your dermatologist a short but useful timeline and makes your visit far more productive. The hair loss dermatologist guide can help you prepare the right questions to ask.
How hair loss is diagnosed: Step-by-step process
Understanding why diagnosis matters so much requires knowing what dermatologists are actually looking for. Hair loss is not one disease; it's a category of conditions that look similar on the surface but require completely different treatment paths. Sending someone with scarring alopecia home with a bottle of minoxidil, for instance, is not just ineffective. It can delay treatment that might have preserved their remaining follicles.
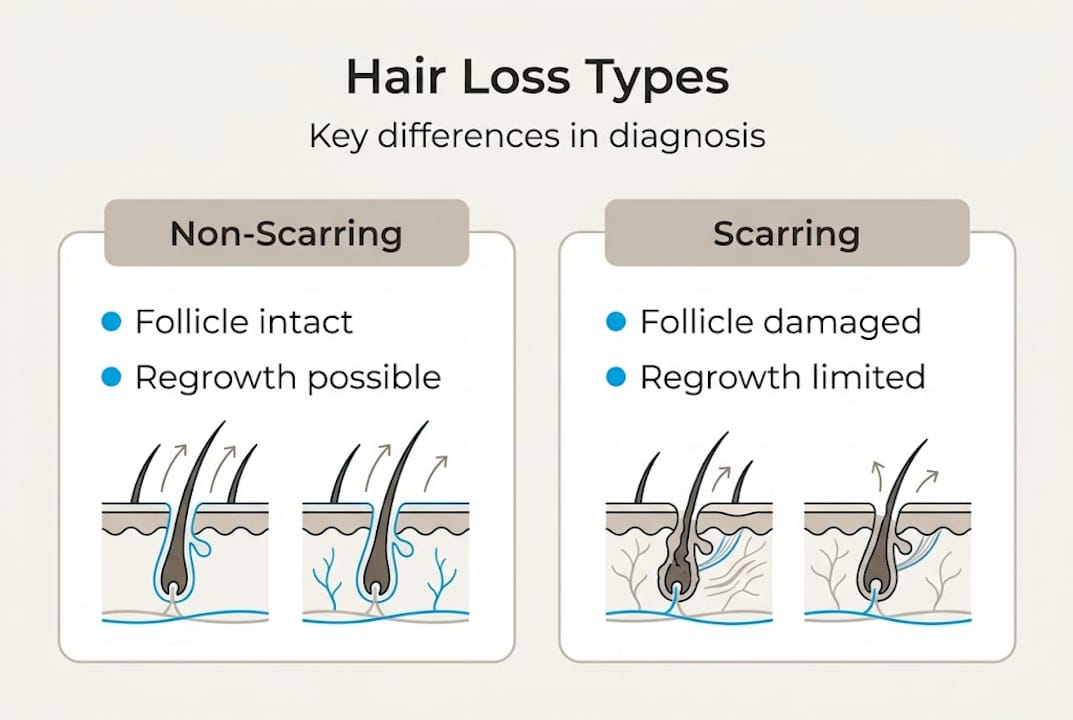
The alopecia classification system separates hair loss into two broad groups: scarring and non-scarring. In non-scarring hair loss, the follicles remain intact and are capable of regrowth. In scarring alopecia (also called cicatricial alopecia), chronic inflammation destroys the follicle permanently and replaces it with fibrous tissue. A biopsy is often essential to catch scarring cases early, especially when the condition looks diffuse or atypical.
Here is how a dermatologist typically moves through the diagnostic process:
- Detailed patient history: When did shedding start? Was it sudden or gradual? Any recent illness, surgery, crash dieting, or major stress? Family history of baldness on both sides is recorded.
- Scalp and hair examination: Pattern mapping, hair density estimation, and checking for signs of inflammation, redness, or pustules.
- Pull test: The dermatologist gently pulls 50 to 60 hairs from multiple scalp zones. More than 10% coming out easily suggests active shedding.
- Trichoscopy: The magnified view reveals whether follicle openings are preserved (non-scarring) or absent and replaced by white fibrosis (scarring).
- Blood panel: This rules out correctable systemic causes like iron deficiency, thyroid dysfunction, or hormonal imbalances.
- Scalp biopsy: If the picture is still unclear, two small punch biopsies are taken and analyzed under a microscope.
| Feature | Non-scarring hair loss | Scarring hair loss |
|---|---|---|
| Follicle status | Intact, capable of regrowth | Permanently destroyed |
| Common examples | Androgenetic alopecia, telogen effluvium | Lichen planopilaris, discoid lupus |
| Biopsy needed | Sometimes | Almost always |
| Urgency of treatment | Moderate | High |
| Regrowth possible | Yes, with treatment | Partial at best |
| Trichoscopy finding | Miniaturized follicles | White fibrosis, absent openings |
Understanding the hair loss treatment process becomes a lot more logical once you know which category your condition falls into. Treatment for telogen effluvium (a temporary, stress-triggered shed) looks nothing like treatment for frontal fibrosing alopecia.
Treatment options: What to expect from a hair dermatologist
Once a clear diagnosis is made, your dermatologist will discuss treatment options tailored to your specific condition, age, and health history. The good news is that evidence-based options have grown significantly in the last decade. The challenging part is that results take time, often three to six months before you see meaningful change, and patience is genuinely required.

Topical and oral medications are the first line of attack for most androgenetic alopecia (the pattern baldness that affects roughly 50% of men and women over 50). Topical minoxidil 5% remains the gold standard for stimulating follicle activity and is effective for both men and women. Oral finasteride 1mg blocks the conversion of testosterone to DHT (dihydrotestosterone, the hormone that shrinks follicles) and is highly effective for men. Among the evidence-based treatments reviewed by experts in 2026, dutasteride 0.5mg showed a net gain of approximately 9.2 hairs per square centimeter compared to placebo, outperforming finasteride in several network meta-analyses.
Procedural options include platelet-rich plasma (PRP) therapy, which involves drawing your blood, spinning it to concentrate growth factors, and injecting it into the scalp. Low-level laser therapy (LLLT), delivered through laser caps or in-office devices, stimulates cellular energy in hair follicles. Both are particularly useful for patients who can't tolerate oral medications or want to combine approaches.
| Treatment type | Common options | Best suited for | Typical onset |
|---|---|---|---|
| Topical | Minoxidil 5% | Androgenetic alopecia, any sex | 3 to 4 months |
| Oral medication | Finasteride, dutasteride | Male pattern baldness | 3 to 6 months |
| Procedural | PRP, LLLT | Multiple types | 4 to 6 months |
| Combination | Minoxidil + finasteride + PRP | Moderate to severe loss | 4 to 8 months |
Factors your dermatologist weighs when choosing a plan include:
- Your age and sex: DHT-blocking medications are not appropriate for women who are pregnant or may become pregnant
- Type and pattern of hair loss: Diffuse loss responds differently than frontal or vertex thinning
- Existing health conditions: Liver function, cardiovascular health, and hormonal status all influence medication choices
- Safety profile preferences: Some patients prefer topical-only approaches; others want faster results with oral therapy
- Combination potential: Research consistently shows that combining a topical agent with an oral medication or a procedural treatment produces better outcomes than any single approach
The best hair regrowth treatments available today are not magic; they work best when matched to your diagnosis. You can also explore hair loss product options to understand which formulations align with clinical recommendations. For a broader look at where the field is heading, innovative hair therapies are expanding what's possible for patients who haven't responded to conventional options.
Targeted solutions for unique types of hair loss
Not everyone's hair loss fits neatly into the androgenetic box. Alopecia areata, for example, is an autoimmune condition where the immune system attacks hair follicles. It can cause patchy loss, total scalp hair loss (alopecia totalis), or complete body hair loss (alopecia universalis). It affects people of all ages and sexes, including children, and requires a completely different treatment strategy.
For alopecia areata, dermatologists have historically used intralesional corticosteroid injections directly into bald patches, achieving roughly 60% improvement in many patients. But the real breakthrough has been JAK inhibitors, a class of drugs that quiet the immune pathway responsible for attacking follicles. Ritlecitinib, one of the newer JAK inhibitors approved specifically for alopecia areata, has shown sustained response rates of 68 to 85% at week 48 in clinical trials. That's a genuinely significant shift in what's possible for patients who previously had few effective options. You can learn more about current alopecia solutions being offered at specialist clinics.
Hair loss types that tend to respond best to targeted, personalized therapy include:
- Alopecia areata: JAK inhibitors, corticosteroids, and combination immunotherapy
- Telogen effluvium: Correcting nutritional deficiencies (ferritin, vitamin D, zinc) and managing the triggering stressor
- Traction alopecia: Lifestyle modification plus topical minoxidil for early-stage cases
- Hormonal hair loss in women: Anti-androgens like spironolactone combined with topical minoxidil
- Scarring alopecia: Anti-inflammatory agents (hydroxychloroquine, tetracyclines) to stop progression as the top priority
Dermatologists also consider lifestyle deeply. A patient with chronic sleep deprivation and high cortisol levels will not respond as well to topical treatments as someone who has addressed their systemic triggers. That's why the consultation feels almost like a full health review, because it often needs to be. Check out the recommended hair loss strategies that dermatologists most commonly pair with clinical treatment, and if you're managing a bald spot specifically, the solutions for bald spots guide covers targeted approaches for the frontal hairline.
Pro Tip: Keep a monthly photo diary of your scalp, taken from the same angle and in the same lighting each time. When you bring these images to your dermatologist, they can spot subtle density changes or regrowth patterns that are easy to miss in person and almost impossible to recall from memory alone.
Our take: Why measuring your hair health is as vital as the right dermatologist
Here's something conventional hair loss advice almost never says: seeing a great dermatologist is only half the equation. The other half is what you do between appointments.
Most patients leave a dermatologist's office with a prescription and a vague instruction to "come back in three months." But three months is a long time to go without any data. You might stop using a product because you don't notice a difference, when in reality subtle regrowth has already begun. Or you might continue a treatment that's causing side effects, unsure whether to push through or stop. The gap between specialist visits is where outcomes are actually won or lost.
AI-powered hair tracking, like what you can access when you track your hair score, gives you something most dermatology appointments can't: continuous, objective measurement. When you bring that data to your next appointment, you're not describing how your hair "feels" or "seems." You're showing your doctor a trend line. That changes the conversation entirely.
Patients who understand their baseline and actively monitor their progress are far more likely to stay consistent with treatment, catch problems early, and achieve their goals. Objective measurement isn't a replacement for specialist care; it's what makes specialist care more effective. Bring your tracking data to every appointment and treat it as a clinical tool, not a personal journal.
Take the next step: Tools and clinics for measurable progress
If you want to apply what you've learned, advanced tools and vetted local clinics can help you move from information to action.
MyHair.ai's AI-powered hair analysis tool gives you an objective baseline of your hair health from your first scan, then tracks change over time with every follow-up. It's not a guess or a general rating; it's a personalized score built from your actual hair patterns. You can take that data directly to your dermatologist or use it to monitor how well your current treatment is working between visits. Ready to connect with a specialist? Use our platform to find clinics near you that are verified and equipped for evidence-based hair loss care. Your next step toward real results starts with one scan.
Frequently asked questions
What tests will my dermatologist use for hair loss?
A hair dermatologist may use a history review, pull test, trichoscopy, blood tests, and sometimes a scalp biopsy to pinpoint your type of hair loss. The diagnostic tools used depend on how complex or ambiguous your case appears at the first visit.
How do I know if I have scarring or non-scarring hair loss?
Only a dermatologist can confirm this with an exam and, if needed, a scalp biopsy, but non-scarring hair loss keeps follicles intact, meaning regrowth is still possible with the right treatment.
Which hair loss treatments really work?
Topical minoxidil, finasteride, and dutasteride have the strongest evidence, especially when combined with procedural options like PRP or low-level laser therapy for more resistant cases.
What is the newest treatment for alopecia areata?
JAK inhibitors like ritlecitinib now show sustained response rates of 68 to 85% at week 48 for alopecia areata, especially when combined with other therapies for faster initial response.
